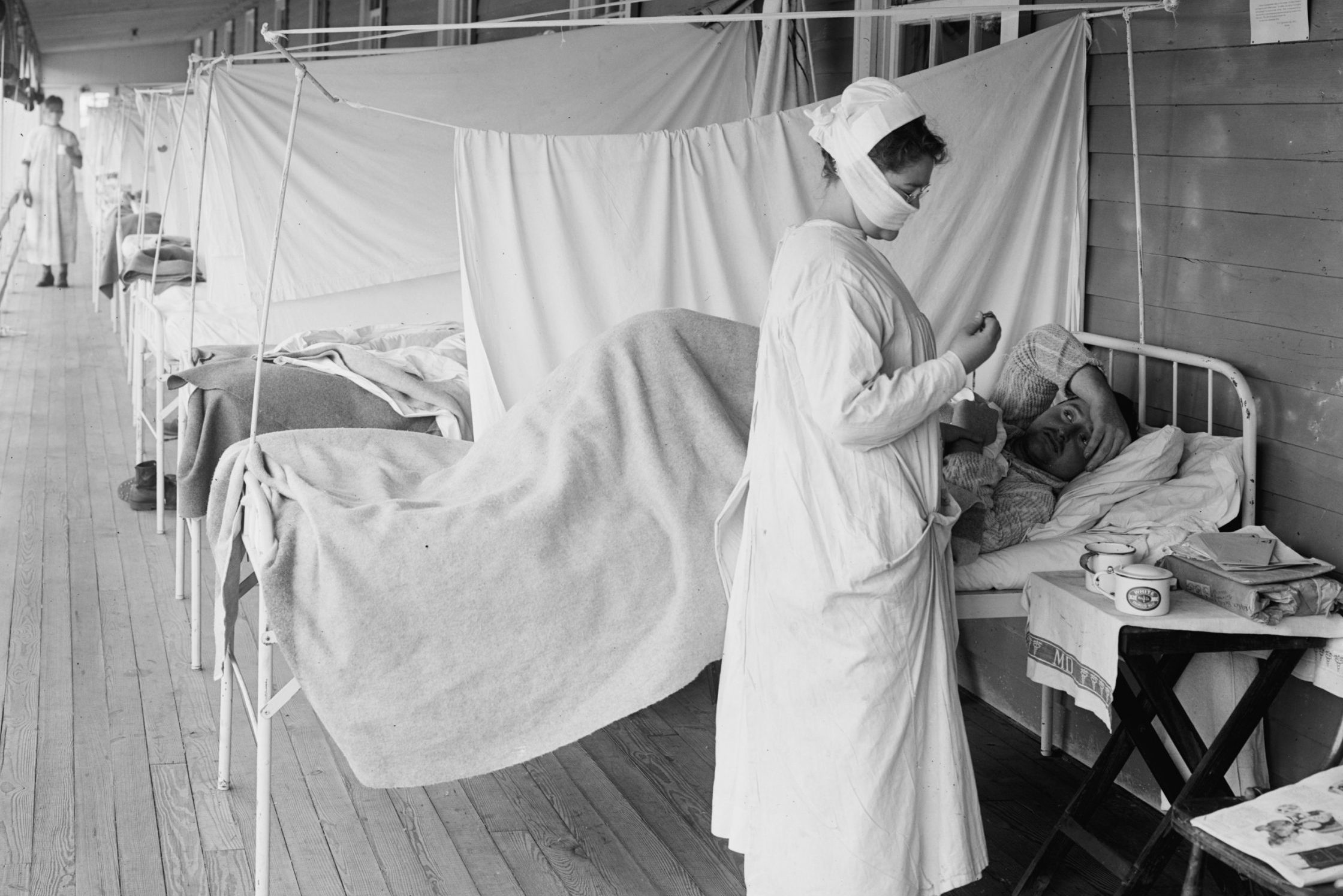
History provides important lessons for the present and future. The pandemic of 1918-19, called the “Spanish Flu” (which originated in the United States), is a good indicator of what we’re currently experiencing, says Gary Green, M.D., a California infectious disease specialist at Sutter Santa Rosa Regional Hospital.
“The world is about one year into this pandemic, as it was in the winter of 1918 during the Spanish Flu, the deadliest pandemic in modern history. The second wave of the Spanish Flu pandemic of 1918-19, which happened right at this same timeframe, fall and winter, was the hammer and the deadliest wave,” says Dr. Green.
Cases grew exponentially then, similarly to what we’re experiencing now.
“That’s what we are seeing with COVID-19 right now,” says Dr. Green. “Most regions are in the second pandemic wave, and it’s been the worst wave so far with historic cases and fatalities, especially for California. That’s why it’s imperative that we take all the safety measures and precautions seriously.”
COVID-19 fatigue is real and understandable after one year of dealing with the virus. But Dr. Green and Bill Carroll, M.D., vice president of medical affairs at Sutter Santa Rosa Regional Hospital, believe there is light at the end of the tunnel.
“We’re on the verge of being able to pull out of [this] as we begin to vaccinate our communities,” Dr. Carroll said.
Dr. Carroll who, along with the rest of the leadership team at Sutter Santa Rosa, helps to support front-line workers as they care for COVID-19 patients, says it’s critical for the public to continue to mask, wash their hands and social distance.
“We’ve been planning since last spring for a surge, but right now is without a doubt the biggest surge we’ve seen since the pandemic began,” Dr. Carroll said.
New Year, New Us?
In the first two weeks of the New Year, California and states across the U.S. are seeing the highest levels of community spread than at any other point during the pandemic.
“We’re seeing an increase in community spread, and when that happens, we’re predictably going to see an increase in the number of patients in the hospital,” Dr. Carroll said.
He explains that the vast majority of people infected with COVID-19 won’t be hospitalized. However, if more people are infected, it’s more likely that some of those individuals are going to get really sick and that some may die, especially when you look at those who are older and those with co-morbid conditions.
Dr. Green agrees.
“When I have a patient in the hospital, I always ask: ‘Who is sick at home?’ What I typically hear is that everyone was sick, and then someone in the family who has medical problems or is older just has never gotten better.”
As people have socialized and traveled during recent holidays, it’s making the situation more dire, especially in cold winter months when people are gathering indoors.
“Once COVID-19 gets into the house, it is difficult to avoid infection in the household,” Dr. Green said. “And often enough one or two in the household end up hospitalized.”
Is the Virus Deadlier?
“We have been tracking and anticipating new strains since the start of this pandemic” says Dr. Green. There are new strains of COVID-19 circulating, one from the UK and one from South Africa, that seem to be more contagious. But Dr. Green points out that they do not seem any more severe or deadly.
“The virus is not becoming more dangerous,” said Dr. Green. “Even though these new strains are more contagious, they are not more severe, so it’s not leading to a higher proportion of severe illness.” Nonetheless, “more people are going to get ill with these more contagious strains if we don’t follow public health recommendations more carefully than ever,” encourages Dr. Green.
The rollout of COVID-19 vaccines to healthcare workers and other prioritized groups is a ray of hope on the horizon.
“We can get through this and we’re getting closer every single day,” said Dr. Carroll.