Meeting people where they are with healthcare can be extremely effective. Digital health capabilities are one obvious example. Community-based efforts also have an impact. Each time, care is accessed more conveniently and delivered from people and in places they trust.
The same concept is now being applied to those working in healthcare. This time, stress relief techniques and support are brought to nurses, technicians and other key staff as they work their shifts inside the hospital.
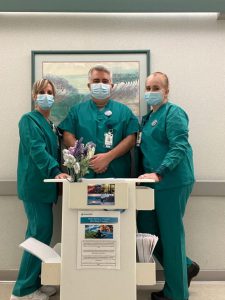
Registered nurses Judy Dean, Arron Buttram and Ginger Luna are part of the Mind-Body program at Memorial Medical Center in Modesto, Calif.
“These past few years have not only impacted healthcare as a whole, but also individual lives,” said Arron Buttram, a registered nurse at Memorial Medical Center in Modesto, Calif. “Anxiety is a human response to such an impact.”
Buttram and his other registered nurse colleagues, Judy Dean and Ginger Luna, have been making specialized rounds inside Memorial Medical Center since August 2021. Known as the Mind-Body team, they come rolling down the hall, touting a utility cart that has been converted to carry aromatherapy packs, mini mandalas for coloring along with other tools and information. They spend four weeks inside a unit emphasizing a particular focus area—“heart,” “mind,” “body” or “connection.” In the theme of each week’s focus, the Mind-Body team lead staff through various integrative medicine techniques. Staff can practice meditation, Reiki, breath work, guided imagery, tapping or even yoga. Depending on the therapy chosen, sessions can take place one-on-one or in groups.

Coloring mandalas are one of the mindfulness practice within the Mind-Body program at Memorial Medical Center in Modesto, Calif.
“A lot of these techniques and therapies were born out of integrative health approaches we use with our cancer patients,” said Rochelle Lonn, a nursing director who helps lead several patient care programs at Memorial Medical Center. “We understood the healing properties of these approaches and immediately thought they could translate to the world of our clinical caregivers.”
Mental health support needs have been growing and have only exploded since COVID-19. And while healthcare systems have invested in efforts offering more support, some of those resources can be only offered offsite or at off times. Bringing the support to them—and showing how they can apply those mindful practices as they enter information into a patient chart or as they prep a patient for discharge—is invaluable.
“I’m grateful to be within a healthcare paradigm that empowers individuals to recognize the specific needs of everyday living that are essential in supporting their innate healing abilities,” said Luna.

Ginger Luna helps Surgical Services Staffing Coordinator, Teresa Cattedra, practice breath work and meditation at Memorial Medical Center, in Modesto, Calif.
Overall, feedback from staff has been very positive. Comments gathered during surveys have ranged from, “It was very soothing and peaceful. I feel so much lighter and calm now,” to “It was magical. It felt good to focus on myself for once.” Surveys also included an informal poll where participants were asked to rate their anxiety levels before and after the program on a scale from 0 to 5. Zero equaled no anxiety and 5 equaled high anxiety. Out of 60 respondents, 35 of them rated their anxiety levels at 3 or higher before the program. Nearly all program participants—59 of them—rated their anxiety at level 2 or less after the program.
So far, the Mind-Body program has visited team members from the intensive care, medical and telemetry units. Any interested staff from other departments is welcome to make requests for the Mind-Body team to visit. The Mind-Body team even return as part of a “rounding week” to see how staff is managing with their new tools and practices.
“Only through first taking time and loving yourself are we able to love and care for others,” said Dean.
Note: This content is not intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.





