The healthcare community has acknowledged how unconscious human bias by individual providers can impact care. Now research reveals how bias embedded within medical technology affects outcomes as well.
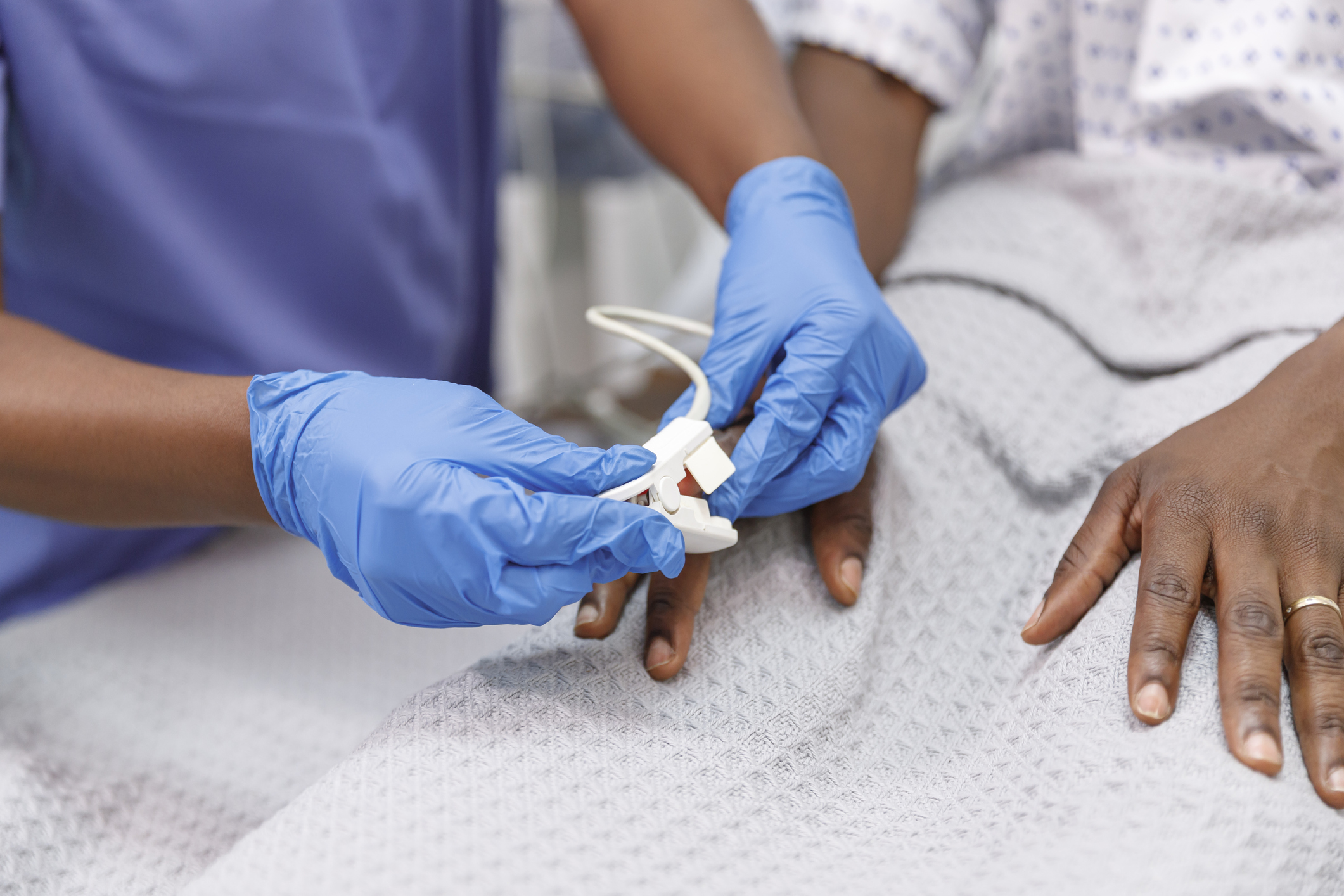
A new study released today by Sutter Health, links medical technology bias to impacts on COVID-19 clinical care. The study found the pulse oximeter’s inability to precisely read the blood oxygen levels of Black patients could have contributed to 4.5-hour treatment delays. The widely used device is placed on a patient’s fingertip and reads blood oxygen level through the skin.
Pulse oximeters were previously found to cause higher error rates in Black patients due to device’s inability to accurately read oxygenation levels on darker skin, revealing a technological bias. A recent JAMA study also revealed how this resulted in lower likelihood for COVID-19 treatment among several ethnicities.
But the length of these delays remained unquantified—until now.

Dr. Stephanie Brown
“The findings underscore the fact that bias is not only human– it can be engrained in the devices and tools clinicians rely on, too,” said Dr. Stephanie Brown, clinical lead for Sutter Health’s Institute for Advancing Health Equity. “To build a more equitable healthcare system we must continue to not only uncover where bias exists in medicine, but also work to understand its impact on clinical outcomes and how it can be corrected. This is good medicine.”
The analysis uncovered that overestimated blood oxygenation was associated with the following delays in COVID-19 care for Black patients:
- Increased time to supplemental oxygen treatment (4.5 hours)
- Increased time to dexamethasone treatment (37 minutes)
- Lower hospital admission probability (3.1%)
- Lower probability of receiving dexamethasone treatment (3.1%)
- Lower probability of receiving supplemental oxygen treatment (4.2%)
The pulse oximeter findings are just the tip of the iceberg. Some of the institute’s additional work includes eliminating the race-based e-GFR calculation throughout the hospitals within its network. Removing this computation can allow for earlier diagnosis and treatment of chronic kidney disease for Black patients. Sutter researchers are also examining how bias impacts algorithms used to assess sepsis, hospital readmissions and palliative care. Dr. Brown said more research and clinical training initiatives around implicit bias continue within the healthcare organization as well. Sutter is partnering with the California Medical Association, Physicians for a Healthy California, the California Primary Care Association and others to host a symposium in October. The goal of the symposium will be to develop evidence-based standards and a framework for unconscious bias training that includes a way to measure their impact and can be implemented across the state.

Kristen Azar
“Our research is just one part of an ongoing, multi-layered process that requires collective action across the healthcare industry to ensure that we are creating targeted interventions that take underrepresented groups into account,” said Kristen M.J. Azar, a registered nurse and scientific medical director of the institute. “By leaning on the benefits of Sutter’s integrated network, our Institute is uniquely positioned to conduct research, analyze data and continue to drive a conversation that precipitates progress in how we practice medicine. Ultimately, our goal is to eliminate health inequities and drive better health outcomes for patients in our network and nationwide.”