Living in a rural community, many miles from a major metropolitan area, has its advantages. But, when you need surgery, the last thing you want to do is take a road trip.
Many rural, community hospitals have physicians that are trained in the surgeries that are often needed. The problem, though, is that the rural hospitals don’t have the equipment for them to perform those surgeries.
A surgeon in Crescent City, a coastal town near the Oregon border, has a plan to provide more minimally invasive and complex procedures for his patients, which will allow them to stay in their hometowns and closer to family and friends.
Along with Sutter Coast Hospital colleagues and hospital leaders, general surgeon Francis Lee, M.D., formed what he calls the SCORE (Sutter Coast Operating Room Equipment) Committee to spearhead efforts to raise the funds necessary to purchase more advanced equipment for Sutter Coast’s surgical department.
The volume of surgical needs has been steadily increasing since he started at Sutter Coast almost three years ago, Dr. Lee says, and he envisions a program that can meet these needs and more without patients ever having to leave their community.
“We can really help this huge population in need,” Dr. Lee says. “I’d like to offer more of what we can do, closer to home. My vision is a comprehensive general surgery program so that we can help a lot more patients than we refer out.”

Dr. Francis Lee created a committee called SCORE to bring advanced surgical tools to rural Sutter Coast Hospital in Crescent City, Calif. “I’d like to offer more of what we can do, closer to home,” he said. “My vision is a comprehensive general surgery program so that we can help a lot more patients than we refer out.”
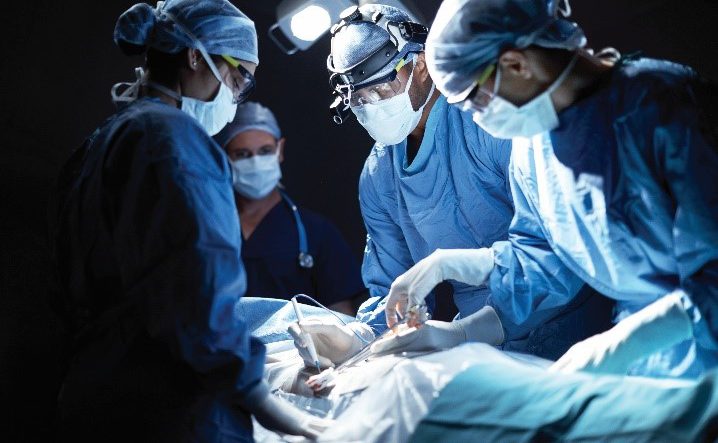
For example, Dr. Lee is well-versed in laparoscopic, minimally invasive surgery. As opposed to “open” surgery, laparoscopic surgeons make much smaller incisions into a patient’s abdomen, which is then inflated with carbon dioxide gas to provide a working and viewing space for the surgeon. The laparoscope transmits images from the area to video monitors in the operating room, images that guide the care team performing the surgery.
By its nature, laparoscopic surgery is associated with less pain, a shorter recovery, fewer post-operative complications and less scarring than traditional open surgeries. Plenty of patients already undergo laparoscopic surgery at Sutter Coast, Dr. Lee says, but cases that require the greatest precision—for example, removing certain types of cancerous growths—have to be referred to hospitals with more advanced equipment, such as ultra-high definition video monitors.
“In our surgery, when we have a much finer detail of the anatomy, it’s safer to operate,” Dr. Lee explains.
Newer laparoscopic equipment and a more advanced X-ray system will likely cost about $500,000 to purchase, by the SCORE Committee’s estimates. Sutter Coast CEO Mitch Hanna has already committed several thousand dollars, as has the Community Assistance League and Dr. Lee’s own family foundation, formed after the death of his 14-year-old son several years ago.
The rest, leaders say, will come from community support, and Sutter Health Philanthropy is matching contributions dollar for dollar. Unlike investor-owned healthcare systems, Sutter Health is a not-for-profit organization: Any money left over after employees and bills have been paid is reinvested in the care of patients and their families.
“Charitable donors are some of our most valuable partners,” Hanna says. “Philanthropy helps makes it possible for our physicians and medical teams to innovate new models of care, recruit new talent, conduct research and, especially important for Sutter Coast right now, purchase advanced technology and expand access to care to our community.”
For more information on how to support these efforts and others, visit sutterhealth.org/giving.